Key points:
- Diabetic neuropathy is the main cause of neuropathies in Mexico.
- Cancer drugs can cause neuropathies, but these can be treated with the support of a neurologist.
- Autonomic neuropathy can pose a risk to the patient’s life, so it must be seen by a doctor.
Peripheral nerve diseases, which include the nerves and nerve ganglia, are known as neuropathies. Dr. Paul Uribe Jaimes, clinical neurologist at ABC Medical Center, says that these types of diseases are very frequent, being a systemic disease, which is related to other conditions such as diabetes, high blood pressure, infections, or even due to the consumption of medications.
To diagnose neuropathy, the doctor must identify whether the symptoms are due to nerve damage or another cause because it is very common to be confused with some other type of disease such as varicose veins, circulatory problems, or other medical problems.
“Peripheral neuropathy, a consequence of damage to the nerves outside the brain and spinal cord (peripheral nerves), often causes weakness, numbness, and pain, usually in the hands and feet. It can also affect other areas and bodily functions, such as digestion, urine, and circulation.”1
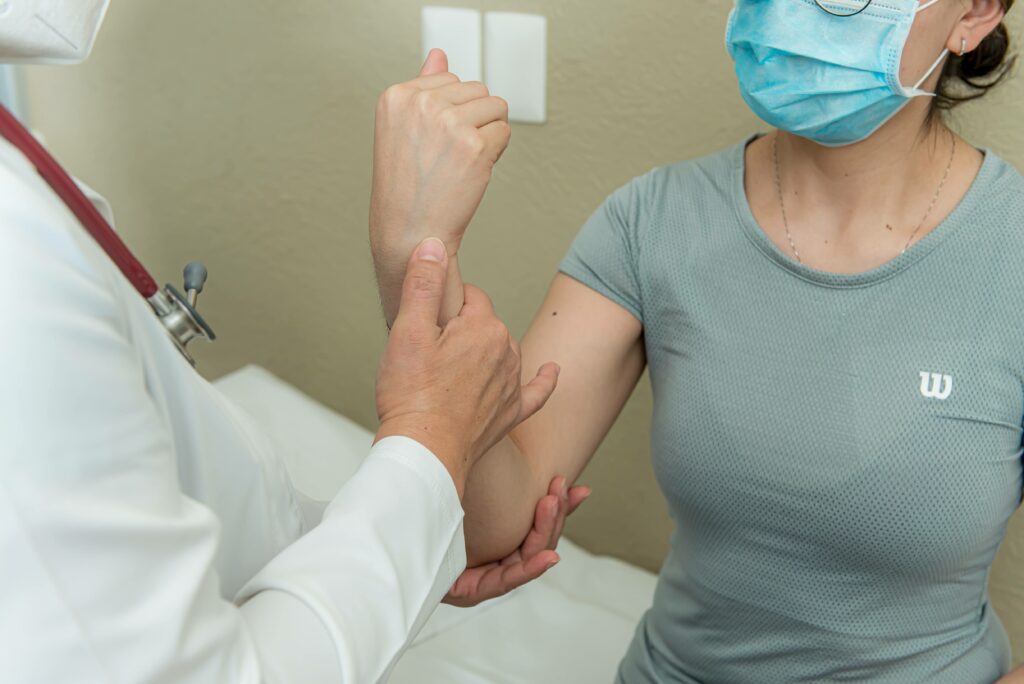
How is a neuropathy assessment performed?
There are some recurring symptoms in cases of neuropathies, these include:
- Changes in feet sensation.
- Tingling, burning, pain, and electric shock sensation.
- Distal weakness in both feet and hand (advanced neuropathy).
If both the patient and the doctor identify the possibility of neuropathy, the doctor will proceed to perform an exam to test the sensitivity of the limbs and the loss of muscle reflexes.
At the same time, they will perform a specialized neurological examination through a deep interrogation related to the symptoms. They will ask questions like, what are you feeling? where do you feel it? at any specific time? Has the feeling changed? Among other questions.
In addition, the doctor can measure your blood pressure in different positions, and your heart rate and its variability during the day and night.
In some very particular cases, that is, in which there is no conclusive information or data and, therefore, there is doubt about the diagnosis, the treating physician may request a more sensitive electrical study.
As these steps are performed, the doctor will identify the type of neuropathy. Dr. Uribe points out that by saying neuropathy, he focuses on any peripheral nerve disease, but beyond that, it must be specifically classified to give it the correct treatment.
Four criteria will be taken for the classifications of neuropathies:
- Topography. Indicates the anatomical areas where the patient perceives the sensations.
- Evolution. Analyzes the duration of the sensations.
- Neurophysiology. Identifies if the problem is in the axon (a part of the cells of the nervous system) or if it is demyelinating (damage to the myelin sheath of nerve fibers).
- Clinic. Tells if the symptoms are motor, sensitive, or autonomic.
To achieve this classification, doctors use body maps in which the patient can indicate everything they feel or perceive, which will allow the disease to be addressed in a specific and non-generic way.
Due to the wide variety of origins of neuropathies, Dr. Uribe indicates three common causes that must be considered:
What is diabetic neuropathy?
There are different causes of neuropathies, in Mexico, having high glucose levels is the most common cause of neuropathy. Studies indicate that up to 15% of patients with diabetes have presented some type of neuropathic symptom. When performing the conduction study in people with diabetes, it has been detected that up to half present data of neuropathies without symptoms.
The reality is that a patient living with diabetes should not suffer from neuropathy and this is achieved by controlling their disease.
On the other hand, it is not mandatory to have diabetes to also have diabetic neuropathy, this is because impaired glucose is a criterion for people who live on the borderline between normal glucose and diabetes, with the possibility of suffering from neuropathy.
What is autonomic neuropathy?
Neuropathies that affect the vital functions of the patient are known as autonomic neuropathy and it is a dangerous disease since it can be life-threatening. This can be detected through tests that measure vital signs such as blood pressure or heart rate in different body positions (standing, lying down, face down, etc.).
Is there neuropathy from chemotherapy?
Chemotherapeutics are a common cause of neuropathies, because, by eradicating tumor cells, secondary damage is caused to nerve neurons. Given this, oncologists are often quite obsessive in detecting whether a patient has neuropathy from chemotherapy. It must be remembered that cancer control is always a priority, says Dr. Uribe, and together, the oncologist and a neurologist can treat the neuropathy.
At ABC Medical Center’s Neurology Center, we can provide you with specialized care. Contact us!
Fuente:
Dr. Paul David Uribe Jaimes – Clinical neurologist and head of neuroscience at ABC Medical Center
https://youtu.be/9eNpaw2cbsc
1https://www.mayoclinic.org/es/diseases-conditions/peripheral-neuropathy/symptoms-causes/syc-20352061