Contact us
Precision Medicine
-
Healthcare Professionals
Healthcare Professionals
Credentialing Requirements
- About ABC
-
Inclusive Health
- ABC Talent
- ABC Foundation I.A.P
- Contact
- ES
What is tavi?
10 November 2025
TAVI, or Transcatheter Aortic Valve Implantation, is a procedure performed when a patient has very advanced stenosis. Aortic stenosis is a common heart disease in which the left ventricle cannot expel blood normally, causing shortness of breath, chest pain, fatigue, or loss of consciousness.
Aortic Valve Implantation
Aortic valve implantation is a procedure performed when the heart’s aortic valve stops functioning properly, either due to stenosis or insufficiency.
Traditionally, this type of surgery requires open-heart intervention, which implies greater risks and a longer recovery time, especially in older people or those with other chronic diseases. But in recent decades, transcatheter aortic valve replacement, or TAVI, has emerged.
The TAVI procedure consists of introducing a new heart valve through a catheter, which usually passes through the femoral artery until it reaches the heart, where it is positioned inside the damaged aortic valve.
This technique allows for valve replacement without the need to open the chest, which results in a lower surgical risk and a faster recovery. The TAVI procedure is usually indicated in patients with severe aortic stenosis who are not ideal candidates for conventional surgery.
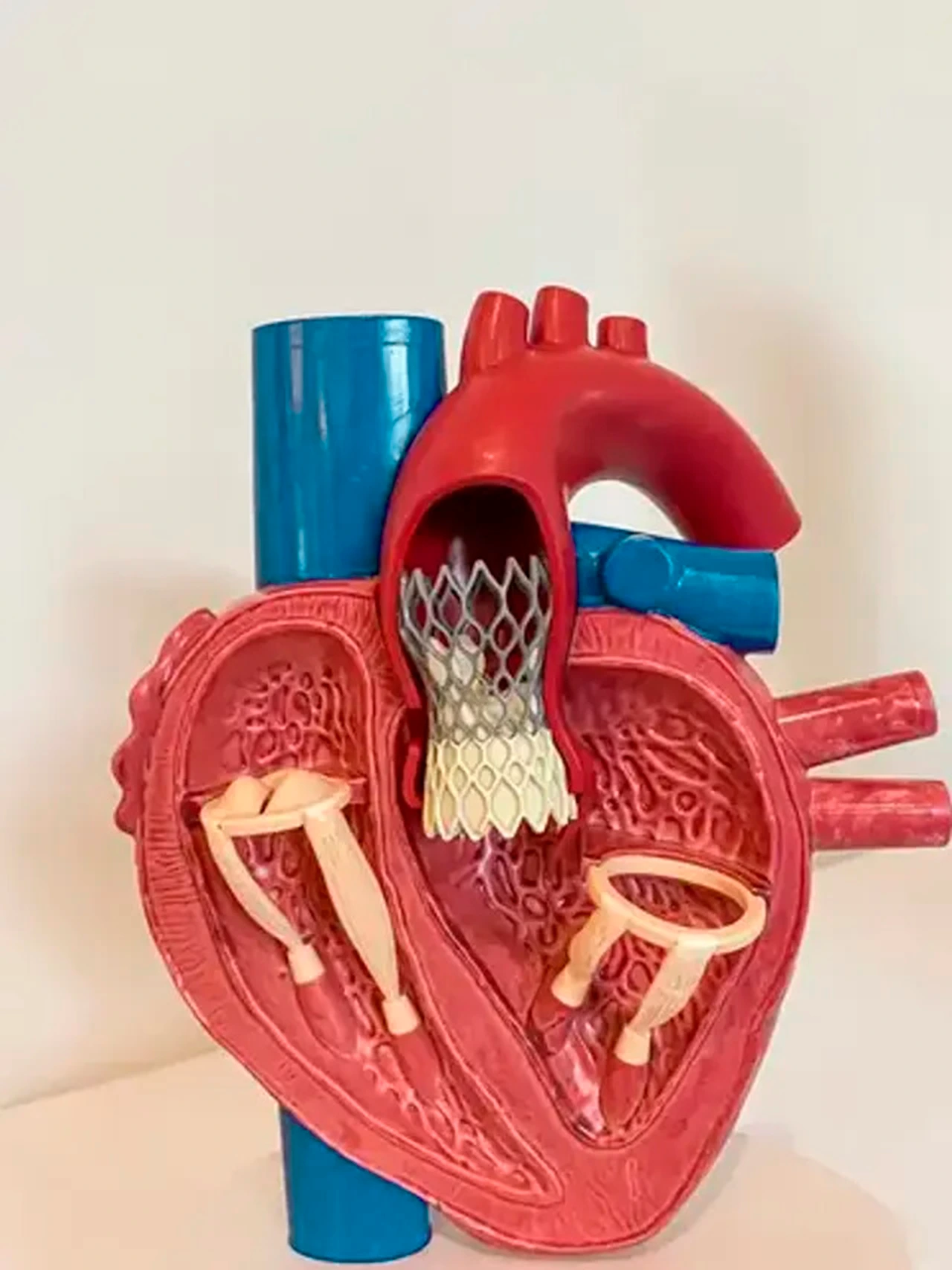
Valvular Stenosis
Aortic valve stenosis is a condition in which the heart’s aortic valve narrows, making it difficult for blood to pass from the left ventricle to the aorta and the rest of the body. This obstruction creates an additional effort for the heart, which over time can result in symptoms such as shortness of breath or chest pain.
This disease usually progresses with age, so it is more common in older adults, and when the stenosis is severe, it becomes a potentially fatal condition if not treated properly.
Very elderly patients or those with diseases that increase the risk of surgery can opt for TAVI. This technique offers a safe and less invasive option. Thanks to this procedure, people who were previously not candidates for surgery can now improve their heart function and regain their quality of life with a more accessible procedure and a faster recovery.
TAVI Complications
Like any other medical procedure, TAVI is not exempt from possible complications. Among the most frequent are bleeding at the catheter insertion site, arrhythmias, the need to place a permanent pacemaker, and, in rare cases, damage to the new valve or stroke.
But all these risks are carefully evaluated before the procedure by a specialized medical team, who are in charge of determining if TAVI is the best option for the patient.
Despite these possible complications, the benefits of TAVI have been shown to greatly outweigh the risks, especially in those patients with severe aortic stenosis and a high surgical risk.
Most patients experience a notable improvement in their symptoms, which translates into a better ability to perform daily activities and, of course, a better quality of life.
At the Cardiovascular Center at ABC Medical Center, we can provide you with specialized care. Contact us!
Fuentes:
How can we help you?

Ricardo Ostos
Content CreatorRicardo can convey complex medical information in an accessible and friendly way so that all of our patients can understand and benefit from it. In addition, he has an empathetic approach, offering information and practical advice that really makes a difference in people's lives. #lifebringsustogether.
Learn more about Ricardo on LinkedIn
Pay in interest-free monthly installments in Specialty Centers, Check Ups, Diagnostic Tests, and Hospitalization
Get from 3 to 9 interest-free installments* with American Express or 6 installments* when paying with Banamex, BBVA, HSBC, Santander or 12 installments*
when paying with Banamex.
Privacy Overview
Error: Contact form not found.
We help you
Send us your request and we will forward it to our specialists. We will get in touch with you very soon.
If you have preferred times to receive our call, please indicate them in your message.
Thank you for contacting us!
Interest-free
months in:
Interest-free
months in:
Specialty Centers
Diagnostic Studies
Check-ups
Hospitalization1
Choose from3 to 9 months when paying with American Express cards 2. Or
6 months when paying with your credit card3 Banamex, BBVA Bancomer, HSBC, Santander.
Or 12 months exclusively when paying with Banamex3
Valid until December 31, 2025. Promotions not cumulative. Subject to restrictions 1. In hospitalization, medical fees are not included. 2. Minimum amount: $1,500 for 3 to 6 months and $3,000 for 7 to 9 months 3. Minimum amount $1,500. (Cards issued abroad are not eligible).
Comparison of COVID-19 vaccines
Pfizer-
BioNTech
Pfizer-BioNTech
What is its effectiveness and what does it refer to?
Vaccine type: mRNA
Effectiveness: 95% after the second dose in the prevention of symptomatic COVID-19.
No Does not contain egg, latex, or preservatives.
How many doses are needed?
Two doses are needed, at least 21 days apart (or up to six weeks apart, if necessary).
Who should or shouldn’t get the vaccine?
People who should receive the vaccine are those over 16 years old.
People who should not receive the vaccine are those who have a history of anaphylactic shock (severe allergy) or who are allergic to any component of this vaccine such as polyethylene glycol (PEG) or polysorbate.
What are the possible side effects of the vaccine?
Pain where the injection was given, fatigue, headache, muscle pain, chills, joint pain, fever, nausea, malaise, and swollen lymph nodes.
How long will it take for me to be protected and what does it protect me from?
After 14 days of having the complete scheme (after the administration of the 2nd dose), the protection period is still under study. It protects us from serious COVID-19 or requiring hospitalization.
Moderna
What is its effectiveness and what does it refer to?
Vaccine type: mRNA
Effectiveness: 94.5% after the second dose in the prevention of symptomatic COVID-19.
Does not contain egg, latex, or preservatives.
How many doses are needed?
Two doses are needed, at least 28 days apart (or up to six weeks apart, if necessary).
Who should or shouldn’t get the vaccine?
People who should receive the vaccine are those over 18 years old.
People who should not receive the vaccine are those who have a history of anaphylactic shock (severe allergy) or who are allergic to any component of this vaccine.
What are the possible side effects of the vaccine?
Pain where the injection was given, fatigue, headache, muscle pain, chills, joint pain, fever, nausea, and swollen lymph nodes in the arm in which you received the injection.
How long will it take for me to be protected and what does it protect me from?
After 14 days of having the complete scheme (after the administration of the 2nd dose), the protection period is still under study. It protects us from serious COVID-19 or requiring hospitalization.
Janssen/
Johnson
& Johnson
Janssen/ Johnson & Johnson
What is its effectiveness and what does it refer to?
Vector-based vaccine.
Effectiveness: 72.0% in the prevention of symptomatic COVID-19.
85% in the prevention of severe COVID-19.
Does not contain egg, latex, or preservatives./strong>
How many doses are needed?
Only one dose in needed.
Who should or shouldn’t get the vaccine?
People who should receive the vaccine are those over 18 years old.
People who should not receive the vaccine are those who have a history of anaphylactic shock (severe allergy) or who are allergic to any component of this vaccine.
What are the possible side effects of the vaccine?
Pain where the injection was given, headache, fatigue, muscle pain, chills, fever, and nausea.
How long will it take for me to be protected and what does it protect me from?
After 28 days of having the complete scheme (the last dose applied), the protection period is still under study. It protects us from 85% serious COVID-19 or requiring hospitalization.
AstraZeneca
and
Oxford
University
AstraZeneca and Oxford University
What is its effectiveness and what does it refer to?
Adenovirus vector-based vaccine.
Effectiveness: 82% after the second dose in the prevention of symptomatic COVID-19.
How many doses are needed?
Two doses are needed, at least 56 days apart (or up to 84 days apart, if necessary).
Who should or shouldn’t get the vaccine?
People who should receive the vaccine are those over 18 years old.
People who should not receive the vaccine are those who have a history of anaphylactic shock (severe allergy) or who are allergic to any component of this vaccine.
What are the possible side effects of the vaccine?
Pain where the injection was given, fatigue, headache, myalgia, arthralgia, and fever, which were mild to moderate in intensity and disappeared within 48 hours of vaccination.
How long will it take for me to be protected and what does it protect me from?
After 14 days of having the complete scheme (after the administration of the 2nd dose), the protection period is still under study. It protects us from serious COVID-19 or requiring hospitalization.
Sputnik V
What is its effectiveness and what does it refer to?
Adenovirus vector-based vaccine.
Effectiveness: 92% after the second dose in the prevention of symptomatic COVID-19.
How many doses are needed?
Two doses are needed, at least 21 days apart (or up to six weeks apart, if necessary).
Who should or shouldn’t get the vaccine?
People who should receive the vaccine are those over 18 years old.
People who should not receive the vaccine are those who have a history of anaphylactic shock (severe allergy) or who are allergic to any component of this vaccine.
What are the possible side effects of the vaccine?
Pain where the injection was given, fatigue, headache, myalgia, arthralgia, and fever, which were mild to moderate in intensity and disappeared within 48 hours of vaccination.
How long will it take for me to be protected and what does it protect me from?
After 14 days of having the complete scheme (after the administration of the 2nd dose), the protection period is still under study. It protects us from serious COVID-19 or requiring hospitalization.
Anti-Herpes Zoster
Herpes zoster is a painful, burning rash. It usually appears on one part of the body and can last for several weeks. It can cause long-lasting severe pain and scarring. Bacterial skin infections, weakness, muscle paralysis, hearing or vision loss may occur less frequently. Herpes zoster is caused by the same virus that causes chickenpox. After you have had chickenpox, the virus that caused it remains in the body of nerve cells. Sometimes after many years, the virus becomes active again and causes herpes zoster.
Vaccination is indicated in the following cases:
- Immunization of patients from 50 years of age for the prevention of herpes zoster and post-herpetic neuralgia (PHN), reduce pain associated with acute or chronic herpes zoster.
Scheme type:
- Single dose.
Rabies
Human rabies is a viral disease transmitted by the bite of an infected animal. It is characterized by acute encephalomyelitis (an aggressive response of the immune system that destroys the myelin layer of the nerves and alters its function at the level of the brain or spinal cord).
Vaccination is indicated in the following cases:
- Prevention of rabies in subjects exposed to risk of contamination. It is recommended for certain international travelers, based on the occurrence of animal rabies in the destination country.
Scheme type:
There are two types.
1. Pre-exposure scheme, consists of three doses of rabies vaccine:
- First dose, on the chosen date.
- Second dose 7 days after the first dose.
- Third dose 28 days after the first dose.
2. Post-exposure scheme, people not vaccinated against rabies, consists of five doses of rabies vaccine.
- First dose, on the date indicated.
- Second dose 3 days after the first dose.
- Third dose 7 days after the first dose.
- Fourth dose 14 days after the first dose.
- Fifth dose 28 days after the first dose.
* If the individual continues to be at risk of exposure to the disease, revaccination should be considered.
Pneumococcal vaccines
Pneumococcal disease can cause serious infections in the lungs (pneumonia), the bloodstream (bacteremia), and the lining of the brain and spinal cord (meningitis).
Two vaccines help prevent pneumococcal disease:
- Pneumoconjugate 13 (pneumococcal conjugate vaccine)
- Pneumococcal 23 (pneumococcal polysaccharide vaccine)
Vaccination is indicated in the following cases:
- Active immunization for the prevention of invasive disease caused by Streptococcus pneumoniae in adults 65 years of age and older.
Scheme type:
- *Two pneumococcal vaccines are recommended for all adults 65 years of age or older.
*One dose of Pneumococcal 13 vaccine should be given first, followed by one dose of Pneumococcal 23 vaccine, depending on your age and health.
